Abstract
Cytolytic activity by CD8+ cytotoxic T lymphocytes (CTLs) is a powerful strategy for the elimination of intracellular pathogens and tumor cells. The destructive capacity of CTLs is progressively dampened during chronic infection, yet the environmental cues and molecular pathways that influence immunological 'exhaustion' remain unclear. Here we found that CTL immunity was regulated by the central transcriptional response to hypoxia, which is controlled in part by hypoxia-inducible factors (HIFs) and the von Hippel–Lindau tumor suppressor VHL. Loss of VHL, the main negative regulator of HIFs, led to lethal CTL-mediated immunopathology during chronic infection, and VHL-deficient CTLs displayed enhanced control of persistent viral infection and neoplastic growth. We found that HIFs and oxygen influenced the expression of pivotal transcription, effector and costimulatory-inhibitory molecules of CTLs, which was relevant to strategies that promote the clearance of viruses and tumors.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Accession codes
References
Via, L.E. et al. Tuberculous granulomas are hypoxic in guinea pigs, rabbits, and nonhuman primates. Infect. Immun. 76, 2333–2340 (2008).
Vaupel, P. Hypoxia in neoplastic tissue. Microvasc. Res. 13, 399–408 (1977).
Eltzschig, H.K. & Carmeliet, P. Hypoxia and inflammation. N. Engl. J. Med. 364, 656–665 (2011).
Rankin, E.B. & Giaccia, A.J. The role of hypoxia-inducible factors in tumorigenesis. Cell Death Differ. 15, 678–685 (2008).
Latif, F. et al. Identification of the von Hippel-Lindau disease tumor suppressor gene. Science 260, 1317–1320 (1993).
Semenza, G.L. HIF-1 and human disease: one highly involved factor. Genes Dev. 14, 1983–1991 (2000).
Nakamura, H. et al. TCR engagement increases hypoxia-inducible factor-1α protein synthesis via rapamycin-sensitive pathway under hypoxic conditions in human peripheral T cells. J. Immunol. 174, 7592–7599 (2005).
Blouin, C.C., Page, E.L., Soucy, G.M. & Richard, D.E. Hypoxic gene activation by lipopolysaccharide in macrophages: implication of hypoxia-inducible factor 1α. Blood 103, 1124–1130 (2004).
Takeda, N. et al. Differential activation and antagonistic function of HIF-α isoforms in macrophages are essential for NO homeostasis. Genes Dev. 24, 491–501 (2010).
Cramer, T. et al. HIF-1α is essential for myeloid cell-mediated inflammation. Cell 112, 645–657 (2003).
Dang, E.V. et al. Control of TH17/Treg balance by hypoxia-inducible factor 1. Cell 146, 772–784 (2011).
Shi, L.Z. et al. HIF1alpha-dependent glycolytic pathway orchestrates a metabolic checkpoint for the differentiation of TH17 and Treg cells. J. Exp. Med. 208, 1367–1376 (2011).
McNamee, E.N., Korns Johnson, D., Homann, D. & Clambey, E.T. Hypoxia and hypoxia-inducible factors as regulators of T cell development, differentiation, and function. Immunol. Res. 55, 58–70 (2013).
Finlay, D.K. et al. PDK1 regulation of mTOR and hypoxia-inducible factor 1 integrate metabolism and migration of CD8+ T cells. J. Exp. Med. 209, 2441–2453 (2012).
Harty, J.T., Tvinnereim, A.R. & White, D.W. CD8+ T cell effector mechanisms in resistance to infection. Annu. Rev. Immunol. 18, 275–308 (2000).
Frebel, H. et al. Programmed death 1 protects from fatal circulatory failure during systemic virus infection of mice. J. Exp. Med. 209, 2485–2499 (2012).
Virgin, H.W., Wherry, E.J. & Ahmed, R. Redefining chronic viral infection. Cell 138, 30–50 (2009).
Matsuzaki, J. et al. Tumor-infiltrating NY-ESO-1-specific CD8+ T cells are negatively regulated by LAG-3 and PD-1 in human ovarian cancer. Proc. Natl. Acad. Sci. USA 107, 7875–7880 (2010).
Baitsch, L. et al. Exhaustion of tumor-specific CD8+ T cells in metastases from melanoma patients. J. Clin. Invest. 121, 2350–2360 (2011).
Wherry, E.J. T cell exhaustion. Nat. Immunol. 12, 492–499 (2011).
Biju, M.P. et al. Vhlh gene deletion induces Hif-1-mediated cell death in thymocytes. Mol. Cell Biol. 24, 9038–9047 (2004).
Haase, V.H., Glickman, J.N., Socolovsky, M. & Jaenisch, R. Vascular tumors in livers with targeted inactivation of the von Hippel-Lindau tumor suppressor. Proc. Natl. Acad. Sci. USA 98, 1583–1588 (2001).
Zhang, D.J. et al. Selective expression of the Cre recombinase in late-stage thymocytes using the distal promoter of the Lck gene. J. Immunol. 174, 6725–6731 (2005).
Gruber, M. et al. Acute postnatal ablation of Hif-2α results in anemia. Proc. Natl. Acad. Sci. USA 104, 2301–2306 (2007).
Ryan, H.E., Lo, J. & Johnson, R.S. HIF-1 alpha is required for solid tumor formation and embryonic vascularization. EMBO J. 17, 3005–3015 (1998).
Wherry, E.J. et al. Molecular signature of CD8+ T cell exhaustion during chronic viral infection. Immunity 27, 670–684 (2007).
Wherry, E.J., Blattman, J.N., Murali-Krishna, K., van der Most, R. & Ahmed, R. Viral persistence alters CD8 T-cell immunodominance and tissue distribution and results in distinct stages of functional impairment. J. Virol. 77, 4911–4927 (2003).
Joshi, N.S. et al. Inflammation directs memory precursor and short-lived effector CD8(+) T cell fates via the graded expression of T-bet transcription factor. Immunity 27, 281–295 (2007).
Kaech, S.M. et al. Selective expression of the interleukin 7 receptor identifies effector CD8 T cells that give rise to long-lived memory cells. Nat. Immunol. 4, 1191–1198 (2003).
Jameson, S.C. & Masopust, D. Diversity in T cell memory: an embarrassment of riches. Immunity 31, 859–871 (2009).
Frauwirth, K.A. & Thompson, C.B. Regulation of T lymphocyte metabolism. J. Immunol. 172, 4661–4665 (2004).
MacIver, N.J., Michalek, R.D. & Rathmell, J.C. Metabolic regulation of T lymphocytes. Annu. Rev. Immunol. 31, 259–283 (2013).
Paley, M.A. et al. Progenitor and terminal subsets of CD8+ T cells cooperate to contain chronic viral infection. Science 338, 1220–1225 (2012).
Oldstone, M.B. Viral persistence. Cell 56, 517–520 (1989).
Medzhitov, R., Schneider, D.S. & Soares, M.P. Disease tolerance as a defense strategy. Science 335, 936–941 (2012).
Nakamoto, N. et al. Synergistic reversal of intrahepatic HCV-specific CD8 T cell exhaustion by combined PD-1/CTLA-4 blockade. PLoS Pathog. 5, e1000313 (2009).
Blackburn, S.D. et al. Coregulation of CD8+ T cell exhaustion by multiple inhibitory receptors during chronic viral infection. Nat. Immunol. 10, 29–37 (2009).
Jin, H.T. et al. Cooperation of Tim-3 and PD-1 in CD8 T-cell exhaustion during chronic viral infection. Proc. Natl. Acad. Sci. USA 107, 14733–14738 (2010).
Snell, L.M., Lin, G.H., McPherson, A.J., Moraes, T.J. & Watts, T.H. T-cell intrinsic effects of GITR and 4–1BB during viral infection and cancer immunotherapy. Immunol. Rev. 244, 197–217 (2011).
Welsh, R.M. Blimp hovers over T cell immunity. Immunity 31, 178–180 (2009).
Intlekofer, A.M. et al. Anomalous type 17 response to viral infection by CD8+ T cells lacking T-bet and eomesodermin. Science 321, 408–411 (2008).
Kaelin, W.G. Jr. Molecular basis of the VHL hereditary cancer syndrome. Nat. Rev. Cancer 2, 673–682 (2002).
Ang, S.O. et al. Disruption of oxygen homeostasis underlies congenital Chuvash polycythemia. Nat. Genet. 32, 614–621 (2002).
Miasnikova, G.Y. et al. The heterozygote advantage of the Chuvash polycythemia VHLR200W mutation may be protection against anemia. Haematologica 96, 1371–1374 (2011).
Niu, X. et al. Altered cytokine profiles in patients with Chuvash polycythemia. Am. J. Hematol. 84, 74–78 (2009).
Tomasic, N.L. et al. The phenotype of polycythemia due to Croatian homozygous VHL (571C>G:H191D) mutation is different from that of Chuvash polycythemia (VHL 598C>T:R200W). Haematologica 98, 560–567 (2013).
Barber, D.L. et al. Restoring function in exhausted CD8 T cells during chronic viral infection. Nature 439, 682–687 (2006).
Doedens, A.L. et al. Macrophage expression of hypoxia-inducible factor-1α suppresses T-cell function and promotes tumor progression. Cancer Res. 70, 7465–7475 (2010).
Lee, P.P. et al. A critical role for Dnmt1 and DNA methylation in T cell development, function, and survival. Immunity 15, 763–774 (2001).
Pircher, H., Burki, K., Lang, R., Hengartner, H. & Zinkernagel, R.M. Tolerance induction in double specific T-cell receptor transgenic mice varies with antigen. Nature 342, 559–561 (1989).
Acknowledgements
We thank members of the Zuniga Laboratory at the University of California, San Diego, for technical advice, discussions and reagents; V. Jhaveri for technical assistance; A. Best for assistance with bioinformatics; the Immunological Genome Project for microarray reagents, processing and assistance; members of the Hedrick Laboratory (University of California, San Diego) for human IL-2 ; and E. Zuniga, S. Hedrick, G. Barton and J. Harker for discussions and review of the manuscript. Supported by the US National Institutes of Health (A.W.G. and R.S.J.), the Pew Scholars Program and the Leukemia Lymphoma Society (A.W.G.), the US National Institutes of Health and University of California, San Diego, Cancer Biology Fund (A.L.D.), the University of California, San Diego, and US National Institutes of Health Cell (A.T.P.) and the Austrian Science Fund (M.H.S.).
Author information
Authors and Affiliations
Contributions
A.L.D. designed and did experiments, analyzed the data and wrote the paper; A.T.P. designed and did experiments, analyzed data and assisted in writing the paper; M.H.S. did histological analysis, provided advice for the design and analysis of pathophysiological experiments and assisted in writing the paper; J.K.F. and J.V.N. did and analyzed viral titer experiments and assisted with animal work; E.Y. did and analyzed immunofluorescence experiments; R.S.J. provided reagents, provided advice for experimental design and wrote the paper; and A.W.G. supervised the project, designed the experiments, analyzed the data and wrote the paper.
Corresponding author
Ethics declarations
Competing interests
A.L.D., A.T.P., R.S.J. and A.W.G. hold a provisional patent for manipulation of the VHL-HIF pathway for therapy.
Integrated supplementary information
Supplementary Figure 1 Deletion of VHL, splenic composition, resting phenotype and TCR responsiveness for the Vhlfl/lf dLck model
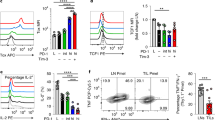
(a) Deletion of VHL in gDNA from sorted CD44lo and CD44hi Vhlfl/fl dLck (VHL-KO) CD8+ T cells relative to WT cells as determined by qPCR, n=2, error bars indicate range. (b) Absolute number of splenic B220+ cells and TCRβ+ cells for wild-type and VHL-KO mice; WT n=6, VHL-KO n=3. * P = 0.014 (Student's unpaired t-test). (c) Representative CD44 and CD62L phenotype of polyclonal CD8+CD4− T cells and the absolute number and relative splenic percentage of indicated subsets; WT n=6, VHL-KO n=3, * P = 0.011, ** P = 0.0011, *** P = 0.033, **** P = 0.023 and ***** P = 0.006 (Student's unpaired t-test). (d) CD127 and KLRG1 phenotype of uninfected splenic polyclonal CD8+CD4− T cells, number and %; n=3, derived from different mice than c; * P = 0.011 (Student's unpaired t-test). (e) CD44 and CD62L phenotype of splenic P14 (CD8α+CD4-Vα2+) T cells from VHL-sufficient and VHL-deficient P14 TCR transgenic mice. (f,g) Equivalent TCR sensitivity/early activation of VHL-sufficient and VHL-deficient P14 T cells to a range of gp33 peptide in vitro and to LCMV clone 13 in vivo. (f) P14 VHL-sufficient or VHL-deficient splenocytes were mixed at a 1:1 ratio and the indicated amount of gp33 peptide was added to duplicate wells. Upregulation of CD69 on VHL-sufficient and VHL-deficient cells was assessed by flow cytometry using congenic markers to distinguish each population after 18 hrs of stimulation; representative of two independent experiments. (g) Experimental set up as in f, but the mixture of P14 CD8+ T cells was transferred into B6 mice followed by infection with LCMV clone 13. Splenocytes were analyzed 36 hrs after infection. Grey-filled histogram indicates the fluorescence of naïve CD8+ T cells from uninfected mice; n=3, representative of two independent experiments. Error bars indicate s.e.m.
Supplementary Figure 2 Similar virus-specific CTL accumulation in T cell–specific triple VHL-HIF-1α-HIF-2α-deficient mice.
Wild-type and VHL-HIF-1α-HIF-2α dLck mice were infected with LCMV clone 13. Frequency of H-2Db gp33 tetramer-positive cells in the peripheral blood for representative samples on day 6 of infection (left) or at the time points indicated (right); n=3, error bars indicate s.e.m., representative of two experiments.
Supplementary Figure 3 VHL-sufficient and VHL-deficient CD8+ T cell response to acute viral infection.
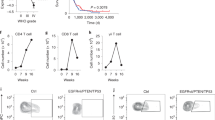
VHL-sufficient and VHL-deficient CD8+ T cell response to acute viral infection. (a) Wild-type or Vhlfl/fl dLck (VHL-KO) mice were infected with LCMV Armstrong and the CD8+ T cell response in peripheral blood was monitored with MHC class I H-2Db gp33 tetramers to detect LCMV-specific CD8+ T cells. Each line indicates an individual mouse; n=6, representative of two experiments. (b-e), A 1:1 mixture of 104 VHL-sufficient and VHL-deficient P14 CD8+ T cells were transferred to B6 hosts followed by infection with LCMV Armstrong one day later; n=3, error bars indicate s.e.m. (b) Experimental scheme. (c) Frequency of transferred VHL-sufficient and VHL-deficient P14 virus-specific cells in peripheral blood as a % of host CD8+ T cells. (d) Absolute number of VHL-sufficient and - deficient P14 splenocytes on day 8 of infection, * P = 0.0002, (Student's unpaired t-test) (e) KLRG1 expression by VHL-sufficient and VHL-deficient P14 cells on day 7 of infection; n=3, * P = 0.007 (Student's unpaired t-test). Results representative of three independent experiments.
Supplementary Figure 4 Inhibitory and exhaustion-associated TIM-3 is increased on VHL-deficient cells and reduced PD-1 expression on VHL-deficient cells is HIF-1α-HIF-2α independent and VHL-dependent.
(a) Cotransfer of VHL-sufficient and VHL-deficient P14 CD8+ T cells followed by LCMV clone 13 infection as in Fig. 2a; histograms of TIM-3 expression and gMFIs of P14 CD8+ T cells from spleen on day 17 of infection with LCMV clone 13; n=4, * P = 0.008 (Student's unpaired t-test). (b) Cotransfer of VHL-sufficient and VHL-deficient P14 CD8+ T cells followed by LCMV clone 13 infection as in Fig. 2a; flow cytometric analysis of splenic VHL-sufficient P14 (black) or VHL-deficient P14 (red) CD8+ T cells at the indicated time points, gMFI shown below. Expression of PD-1 on total host CD8α+ T cells excluding P14 donor cells (histograms, grey), or gMFI for PD-1 low –expressing cells (in graphs, open bars) shown for reference; n=3, * P = 0.004, ** P = 0.05 and *** P = 0.004 (Student's unpaired t-test). (c) Experimental design for a mixed transfer of VHL-sufficient, VHL-deficient and VHL-HIF-1α-HIF-2α-triple-deficient P14 CD8+ donor cells. (d) Histogram of each donor population displaying PD-1 (left) and gMFI graphed (right); peripheral blood on day 7 of infection; n=3, error bars indicate s.e.m.
Supplementary Figure 5 Similar plasma cytokine levels in wild-type and Vhlfl/fl dLck mice responding to persistent infection and in vitro and in vivo cytotoxicity assays of VHL-sufficient and VHL-deficient cells responding to persistent infection.
(a) Plasma cytokine levels in uninfected, polyclonal wild-type, or polyclonal Vhlfl/fl dLck on day 6 of infection with LCMV clone 13; uninfected n=2, wild-type n=5, Vhlfl/fl dLck n = 4; error bars indicate s.e.m. Cytokine levels were determined using Milliplex 32-plex premixed magnetic cytokine array and Luminex bead reader according to the manufacturers instructions. (b) In vitro cytotoxicity assay: VHL-sufficient P14 (here designated as WT) or VHL-deficient P14 T cells (VHL-KO) were transferred into B6 hosts that were then infected with LCMV clone 13 as in Fig. 1a. Splenocytes from hosts harboring VHL-sufficient or VHL-deficient P14 cells were enriched for CD8+ cells on day 7 of LCMV clone 13 infection. Whole splenocytes from an uninfected mouse were used as targets; cells were coated with gp33-41 peptide (KAVYNFATC) at 1μm for one hour, labeled with 5μm of eFluor670 and mixed 1:1 with splenocytes labeled with 250nM of eFluor670. Appropriate numbers of VHL-sufficient or VHL-deficient P14 T cells were added to achieve effector to target ratios indicated, incubated with target cells for 4 hrs, and then assayed by flow cytometry. (c) In vivo cytotoxicity assay: VHL-sufficient versus VHL-deficient P14 T cells were transferred into B6 hosts and infected with LCMV clone 13. Whole splenocytes coated with or without gp33 peptide and eFluor670 labeled as in b, 2.5 × 106 gp33 peptide coated cells per mouse were injected iv 16 days after infection. One hour after injection of target cell mix, splenocytes were isolated from host mice and assayed by flow cytometry. The absolute number of cells binding H-2Db gp33 tetramer (top), the % killing of target cells (middle) and the approximate killing per antigen-specific CD8+ T cell (bottom) are shown. To calculate targets killed per antigen-specific cell: the number of peptide-coated cells transferred to the infected host mouse was multiplied by the % killed to obtain an estimate of absolute number killed. The absolute number of target cells killed was then divided by the number of H-2Db gp33 tetramer+ CD8+ T cells per host spleen to approximate killing per cell. * P = 0.003, ** P = 0.05 and *** P = 0.007 (Student's unpaired t-test). Error bars indicate s.e.m. for all plots.
Supplementary Figure 6 Comparison of established “exhaustion gene-expression profile” with VHL-deficient-expression profile shows significant correlation, but identifies differently expressed genes.
(a) Flow chart of analysis. (a) Flow chart of analysis. (b) Fold-change versus P-value plot of VHL-deficient versus VHL-sufficient P14 cells at day 7 post-infection (data from Fig. 3a). Genes that were reported1 to be upregulated in wild-type exhausted versus wild-type effector cells are highlighted in red, those down in blue; selected genes are identified. Genes up- or downregulated in VHL-deficient versus VHL-sufficient P14 cells show significant correlation with the genes previously reported to be up- or downregulated with exhausted versus effector cells (P = 0.0008 and 0.0004, respectively); Chi-squared test assuming equal distribution of genes up- and downregulated for the VHL-deficient versus VHL-sufficient and exhausted versus effector comparisons. (c) Bar graph representation of the data in a,b identifying the 64 genes that were upregulated in exhausted versus effector CTL; fold-change for VHL-deficient versus VHL-sufficient P14 cells is plotted. (d) As in c, but the fold-change expression of VHL-deficient versus VHL-sufficient of the 109 genes identified in a,b as being downregulated in exhausted versus effector cells.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–6 (PDF 5144 kb)
Rights and permissions
About this article
Cite this article
Doedens, A., Phan, A., Stradner, M. et al. Hypoxia-inducible factors enhance the effector responses of CD8+ T cells to persistent antigen. Nat Immunol 14, 1173–1182 (2013). https://doi.org/10.1038/ni.2714
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni.2714
This article is cited by
-
Human colorectal cancer: upregulation of the adaptor protein Rai in TILs leads to cell dysfunction by sustaining GSK-3 activation and PD-1 expression
Cancer Immunology, Immunotherapy (2024)
-
Focus on T cell exhaustion: new advances in traditional Chinese medicine in infection and cancer
Chinese Medicine (2023)
-
Identification of co-expressed gene networks promoting CD8+ T cell infiltration and having prognostic value in uveal melanoma
BMC Ophthalmology (2023)
-
Mechanisms of HIF-driven immunosuppression in tumour microenvironment
Journal of the Egyptian National Cancer Institute (2023)
-
Hypoxia drives CD39-dependent suppressor function in exhausted T cells to limit antitumor immunity
Nature Immunology (2023)