Abstract
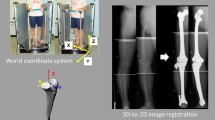
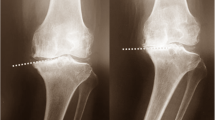
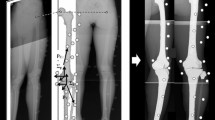
Malalignment is known to affect the medial-to-lateral load distribution in the tibiofemoral joint. In this longitudinal study, we test the hypothesis that subchondral bone surface areas functionally adapt to the load distribution in malaligned knees. Alignment (hip–knee–ankle angle) was measured from full limb films in 174 participants with knee osteoarthritis. Coronal magnetic resonance images were acquired at baseline and 26.6 ± 5.4 months later. The subchondral bone surface area of the weight-bearing tibiofemoral cartilages was segmented, with readers blinded to the order of acquisition. The size of the subchondral bone surface areas was computed after triangulation by proprietary software. The hip–knee–ankle angle showed a significant correlation with the tibial (r 2 = 0.25, P < 0.0001) and femoral (r 2 = 0.07, P < 0.001) ratio of medial-to-lateral subchondral bone surface area. In the tibia, the ratio was significantly different between varus (1.28:1), neutral (1.18:1), and valgus (1.13:1) knees (analysis of variance [ANOVA]; P < 0.00001). Similar observations were made in the weight-bearing femur (0.94:1 in neutral, 0.97.1 in varus, 0.91:1 in valgus knees; ANOVA P = 0.018). The annualized longitudinal increase in subchondral bone surface area was significant (P < 0.05) in the medial tibia (+0.13%), medial femur (+0.26%), and lateral tibia (+0.19%). In the medial femur, the change between baseline and follow-up was significantly different (ANOVA; P = 0.020) between neutral, varus, and valgus knees, with the increase in surface area being significantly greater (P = 0.019) in varus than in neutral knees. Tibiofemoral subchondral bone surface areas are shown to be functionally adapted to the medial-to-lateral load distribution. The longitudinal findings indicate that this adaptational process may continue to take place at advanced age.




Similar content being viewed by others
References
Carter DR, Wong M, Orr TE (1991) Musculoskeletal ontogeny, phylogeny, and functional adaptation. J Biomech 24(suppl 1):3–16
Darwin C (1872) The origin of species. New American Library, New York
Lamarck JB (1809) Philosophie zoologique. Baillere, Paris
Roux W (1881) Der Kampf der Teile im Organismus. Engelmann, Leipzig
Wolff J (1892) Das Gesetz der Transformation der Knochen. Hirschwald, Berlin
Booth FW (1994) Terrestrial applications of bone and muscle research in microgravity. Adv Space Res 14:373–376
Keller TS, Strauss AM, Szpalski M (1992) Prevention of bone loss and muscle atrophy during manned space flight. Microgravity Q 2:89–102
Huiskes R, Ruimerman R, van Lenthe GH, Janssen JD (2000) Effects of mechanical forces on maintenance and adaptation of form in trabecular bone. Nature 405:704–706
Andriacchi TP (1994) Dynamics of knee malalignment. Orthop Clin North Am 25:395–403
Cooke TD, Sled EA, Scudamore RA (2007) Frontal plane knee alignment: a call for standardized measurement. J Rheumatol 34:1796–1801
Johnson F, Leitl S, Waugh W (1980) The distribution of load across the knee. A comparison of static and dynamic measurements. J Bone Joint Surg Br 62:346–349
Maquet P (1979) Mechanics and osteoarthritis of the patellofemoral joint. Clin Orthop Relat Res 144:70–73
Morrison JB (1970) The mechanics of the knee joint in relation to normal walking. J Biomech 3:51–61
Tetsworth K, Paley D (1994) Malalignment and degenerative arthropathy. Orthop Clin North Am 25:367–377
Hurwitz DE, Sumner DR, Andriacchi TP, Sugar DA (1998) Dynamic knee loads during gait predict proximal tibial bone distribution. J Biomech 31:423–430
Müller-Gerbl M (1998) The subchondral bone plate. Adv Anat Embryol Cell Biol 141:III–XI, 1–134
Thorp LE, Wimmer MA, Block JA, Moisio KC, Shott S, Goker B, Sumner DR (2006) Bone mineral density in the proximal tibia varies as a function of static alignment and knee adduction angular momentum in individuals with medial knee osteoarthritis. Bone 39:1116–1122
Lieberman DE, Devlin MJ, Pearson OM (2001) Articular area responses to mechanical loading: effects of exercise, age, and skeletal location. Am J Phys Anthropol 116:266–277
Plochocki JH, Riscigno CJ, Garcia M (2006) Functional adaptation of the femoral head to voluntary exercise. Anat Rec A Discov Mol Cell Evol Biol 288:776–781
Plochocki JH (2004) Bilateral variation in limb articular surface dimensions. Am J Hum Biol 16:328–333
Lazenby RA, Cooper DM, Angus S, Hallgrimsson B (2008) Articular constraint, handedness, and directional asymmetry in the human second metacarpal. J Hum Evol 54:875–885
Eckstein F, Faber S, Muhlbauer R, Hohe J, Englmeier KH, Reiser M, Putz R (2002) Functional adaptation of human joints to mechanical stimuli. Osteoarthritis Cartilage 10:44–50
Buckland WrightC (1995) Protocols for precise radio-anatomical positioning of the tibiofemoral and patellofemoral compartments of the knee. Osteoarthritis Cartilage 3(suppl A):71–80
Moreland JR, Bassett LW, Hanker GJ (1987) Radiographic analysis of the axial alignment of the lower extremity. J Bone Joint Surg Am 69:745–749
Eckstein F, Burstein D, Link TM (2006) Quantitative MRI of cartilage and bone: degenerative changes in osteoarthritis. NMR Biomed 19:822–854
Eckstein F, Charles HC, Buck RJ, Kraus VB, Remmers AE, Hudelmaier M, Wirth W, Evelhoch JL (2005) Accuracy and precision of quantitative assessment of cartilage morphology by magnetic resonance imaging at 3.0T. Arthritis Rheum 52:3132–3136
Eckstein F, Cicuttini F, Raynauld JP, Waterton JC, Peterfy C (2006) Magnetic resonance imaging (MRI) of articular cartilage in knee osteoarthritis (OA): morphological assessment. Osteoarthritis Cartilage 14(suppl 1):46–75
Graichen H, Eisenhart-Rothe R, Vogl T, Englmeier KH, Eckstein F (2004) Quantitative assessment of cartilage status in osteoarthritis by quantitative magnetic resonance imaging: technical validation for use in analysis of cartilage volume and further morphologic parameters. Arthritis Rheum 50:811–816
Eckstein F, Ateshian G, Burgkart R, Burstein D, Cicuttini F, Dardzinski B, Gray M, Link TM, Majumdar S, Mosher T, Peterfy C, Totterman S, Waterton J, Winalski CS, Felson D (2006) Proposal for a nomenclature for magnetic resonance imaging based measures of articular cartilage in osteoarthritis. Osteoarthritis Cartilage 14:974–983
Eckstein F, Hudelmaier M, Wirth W, Kiefer B, Jackson R, Yu J, Eaton CB, Schneider E (2006) Double echo steady state magnetic resonance imaging of knee articular cartilage at 3 Tesla: a pilot study for the Osteoarthritis Initiative. Ann Rheum Dis 65:433–441
Eckstein F, Kunz M, Hudelmaier M, Jackson R, Yu J, Eaton CB, Schneider E (2007) Impact of coil design on the contrast-to-noise ratio, precision, and consistency of quantitative cartilage morphometry at 3 Tesla: a pilot study for the osteoarthritis initiative. Magn Reson Med 57:448–454
Burgkart R, Glaser C, Hyhlik-Durr A, Englmeier KH, Reiser M, Eckstein F (2001) Magnetic resonance imaging-based assessment of cartilage loss in severe osteoarthritis: accuracy, precision, and diagnostic value. Arthritis Rheum 44:2072–2077
Burgkart R, Glaser C, Hinterwimmer S, Hudelmaier M, Englmeier KH, Reiser M, Eckstein F (2003) Feasibility of T and Z scores from magnetic resonance imaging data for quantification of cartilage loss in osteoarthritis. Arthritis Rheum 48:2829–2835
Glaser C, Burgkart R, Kutschera A, Englmeier KH, Reiser M, Eckstein F (2003) Femoro-tibial cartilage metrics from coronal MR image data: technique, test–retest reproducibility, and findings in osteoarthritis. Magn Reson Med 50:1229–1236
Miyazaki T, Wada M, Kawahara H, Sato M, Baba H, Shimada S (2002) Dynamic load at baseline can predict radiographic disease progression in medial compartment knee osteoarthritis. Ann Rheum Dis 61:617–622
Hurwitz DE, Ryals AB, Case JP, Block JA, Andriacchi TP (2002) The knee adduction moment during gait in subjects with knee osteoarthritis is more closely correlated with static alignment than radiographic disease severity, toe out angle and pain. J Orthop Res 20:101–107
Jones G, Ding C, Scott F, Glisson M, Cicuttini F (2004) Early radiographic osteoarthritis is associated with substantial changes in cartilage volume and tibial bone surface area in both males and females. Osteoarthritis Cartilage 12:169–174
Wang Y, Wluka AE, Cicuttini FM (2005) The determinants of change in tibial plateau bone area in osteoarthritic knees: a cohort study. Arthritis Res Ther 7:R687–R693
Wang Y, Ding C, Wluka AE, Davis S, Ebeling PR, Jones G, Cicuttini FM (2006) Factors affecting progression of knee cartilage defects in normal subjects over 2 years. Rheumatology (Oxford) 45:79–84
Eckstein F, Buck RJ, Burstein D, Charles HC, Crim J, Hudelmaier M, Hunter D, Hutchins G, Jackson C, Byers Kraus V, Lane NE, Link TM, Majumdar S, Mazzuca S, Prasad PV, Schnitzer TJ, Taljanovic MS, Vaz A, Wyman B, Hellio Le Graverand MP (2008) Precision of 3.0 Tesla quantitative magnetic resonance imaging of cartilage morphology in a multi center clinical trial. Ann Rheum Dis 67:1683–1688
Sigurdsson G, Aspelund T, Chang M, Jonsdottir B, Sigurdsson S, Eiriksdottir G, Gudmundsson A, Harris TB, Gudnason V, Lang TF (2006) Increasing sex difference in bone strength in old age: The Age, Gene/Environment Susceptibility—Reykjavik study (AGES-REYKJAVIK). Bone 39:644–651
Riggs BL, Melton ILIII, Robb RA, Camp JJ, Atkinson EJ, Peterson JM, Rouleau PA, McCollough CH, Bouxsein ML, Khosla S (2004) Population-based study of age and sex differences in bone volumetric density, size, geometry, and structure at different skeletal sites. J Bone Miner Res 19:1945–1954
Wluka AE, Wang Y, Davis SR, Cicuttini FM (2005) Tibial plateau size is related to grade of joint space narrowing and osteophytes in healthy women and in women with osteoarthritis. Ann Rheum Dis 64:1033–1037
Zhai G, Ding C, Cicuttini F, Jones G (2007) A longitudinal study of the association between knee alignment and change in cartilage volume and chondral defects in a largely non-osteoarthritic population. J Rheumatol 34:181–186
Hunter DJ, Zhang Y, Niu J, Tu X, Amin S, Goggins J, LaValley M, Guermazi A, Gale D, Felson DT (2005) Structural factors associated with malalignment in knee osteoarthritis: the Boston osteoarthritis knee study. J Rheumatol 32:2192–2199
Brouwer GM, van Tol AW, Bergink AP, Belo JN, Bernsen RM, Reijman M, Pols HA, Bierma-Zeinstra SM (2007) Association between valgus and varus alignment and the development and progression of radiographic osteoarthritis of the knee. Arthritis Rheum 56:1204–1211
Hunter DJ, Niu J, Felson DT, Harvey WF, Gross KD, McCree P, Aliabadi P, Sack B, Zhang Y (2007) Knee alignment does not predict incident osteoarthritis: the Framingham osteoarthritis study. Arthritis Rheum 56:1212–1218
Acknowledgments
We thank Pottumarthi Prasad for his help with the image acquisition and Wolfgang Hitzl, Research Office of Paracelsus Medical University, for his help with the statistical analysis. We would also like to thank the following readers for their help with subchondral bone surface segmentation: Julia Bula-Sternberg, Gudrun Goldmann, Linda Jakobi, Verena Lengfelder, Ilona Lipp, Manuela Kunz, Dr. Susanne Maschek, Sabine Mühlsimer, Franz Romeder, Verena Stein, Annette Thebis, and Dr. Barbara Wehr. We thank NIH/NIAMS for funding this study through the following grants: RO1 AR48216, RO1 AR48748, P60 AR48098.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Eckstein, F., Hudelmaier, M., Cahue, S. et al. Medial-to-Lateral Ratio of Tibiofemoral Subchondral Bone Area is Adapted to Alignment and Mechanical Load. Calcif Tissue Int 84, 186–194 (2009). https://doi.org/10.1007/s00223-008-9208-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00223-008-9208-4